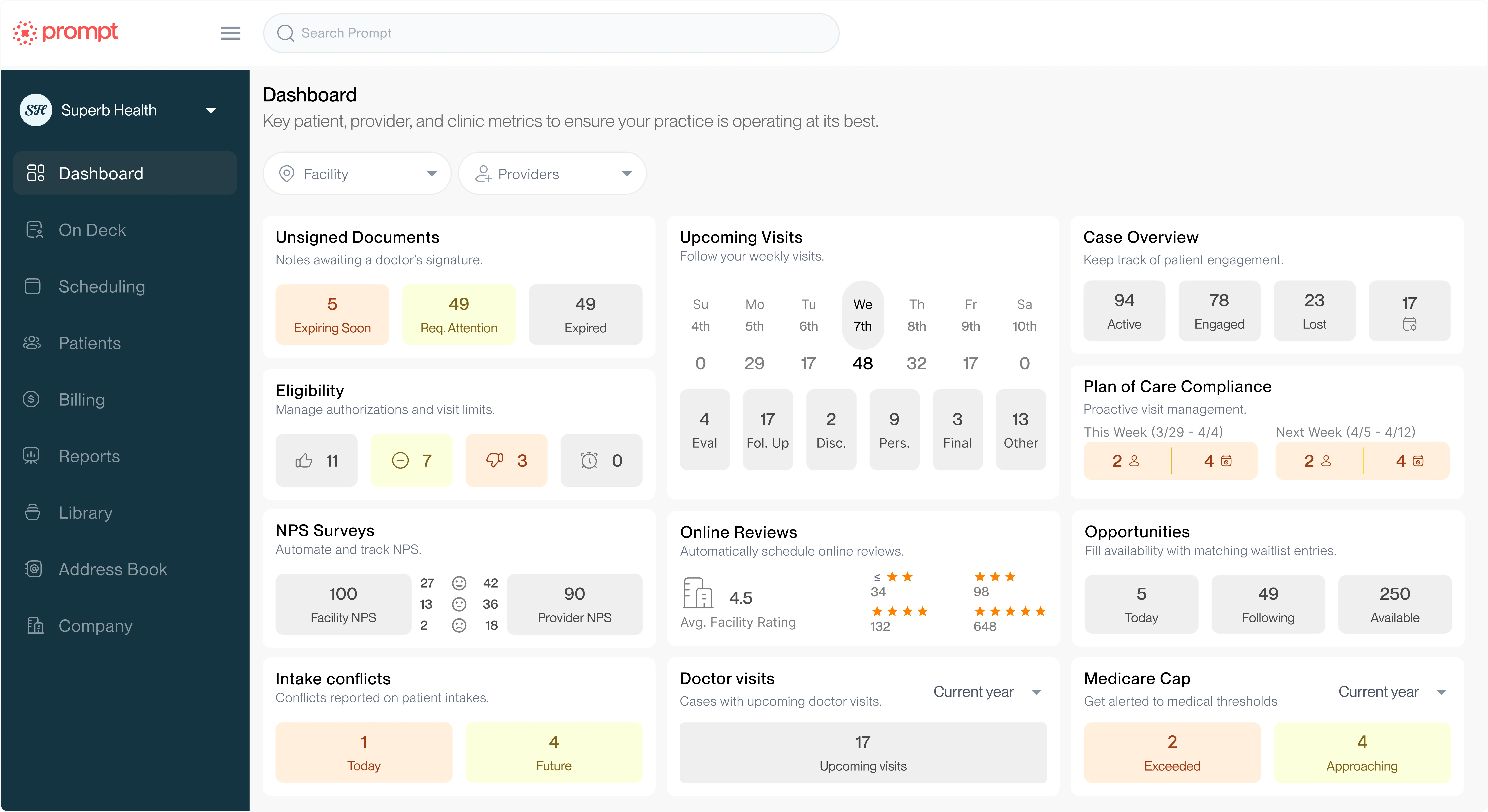
AI tools in physical therapy are engineered to reduce the administrative burden that constrains clinic operations and limits sustainable growth. The most widely adopted applications in practice include AI scribes for clinical documentation, predictive analytics for billing denial prevention, and automated scheduling systems that fill open appointment slots while reducing patient no-shows and drop-offs.
The administrative load on PT clinics is both substantial and empirically documented through peer-reviewed research and industry surveys. According to APTA's 2025 Administrative Burden Report, 75% of physical therapy providers have had to hire additional administrative staff to keep up with escalating payer requirements.
That same report found an average of 12.9% of PT claims are denied by payers, creating a systematic drag on clinic revenue. Nearly one in three physical therapists now wait one to two weeks for prior authorization approval, a figure that has increased 9 percentage points since APTA's prior survey cycle.
Effective AI implementation in rehabilitation hinges on transparency, clinical accuracy, and seamless integration with established workflows. Tools like Prompt are purpose-built to support clinicians rather than replace clinical judgment, which is the foundational framework for responsible AI adoption in physical therapy.
Why it matters
AI enables clinics to scale their operations without proportionally increasing administrative headcount or overhead costs. It directly addresses the well-documented burnout crisis in rehabilitation by reducing "pajama time," the widely used industry term for the hours clinicians spend completing documentation outside of normal business hours.
The scope of this crisis has been demonstrated through multiple peer-reviewed studies and verified by professional organizations. A 2023 study published in the Journal of Educational Evaluation for Health Professions, highlighted by the American Physical Therapy Association, found that nearly 50% of physical therapists surveyed reported experiencing clinical burnout.
APTA's own systematic administrative burden research reinforces this finding: 85% of physical therapists report that prior authorization requirements negatively affect their patients' clinical outcomes, and 83% say prior authorization has directly caused patients to abandon their established treatment plans entirely.
No-shows compound the operational strain on clinics that are already stretched thin by administrative demands. A 2021 retrospective cohort study published in PLOS ONE, analyzing data from 444,995 physical therapy patients across 828 clinics in 26 states, found that 73% of patients missed at least one scheduled appointment during their care episode.
In practical terms, this means PT clinics routinely lose scheduled treatment slots they cannot recapture, resulting in both direct revenue gaps and measurable interruptions in patient care continuity.
AI-powered scheduling and automated patient outreach help clinics systematically reclaim those lost visits while freeing front-desk staff from manual follow-up responsibilities.
Key applications of AI in physical therapy
The following represent the most established, evidence-supported use cases for AI in outpatient PT clinic operations today.
AI scribes for clinical documentation
Ambient listening tools transcribe clinician-patient conversations and generate structured clinical notes in real time during the encounter. The clinician reviews and signs every note, maintaining full clinical oversight throughout the entire documentation process. This methodology ensures that AI accelerates documentation without compromising the clinical evidence standard.
Peer-reviewed evidence from broader healthcare settings demonstrates the proven potential of this technology for rehabilitation professionals:
- A multi-center quality improvement study published in JAMA Network Open, conducted across six U.S. health systems with 263 clinicians in 2024, found that after 30 days with ambient AI scribes, clinician burnout dropped from 51.9% to 38.8%, representing 74% lower odds of burnout after just one month of consistent use.
- In a separate analysis published in NEJM Catalyst, The Permanente Medical Group reported that AI scribes saved an estimated 15,791 hours of documentation time across 2.5 million patient encounters, which is equal to roughly 1,794 eight-hour workdays of recovered clinician capacity.
- A 2025 allied health study published in Musculoskeletal Science and Practice demonstrated that clinician productivity increased by an average of 5.8% when using an AI scribe, with participants reporting independently verified positive effects on both therapeutic alliance and administrative workload reduction.
While the JAMA and NEJM studies reflect broader healthcare settings rather than PT-specific data, the documentation burden they address is shared across all rehabilitation disciplines.
Predictive billing analytics
Machine learning models analyze historical claim data, payer-specific rules, and documentation patterns to flag likely denials before claim submission occurs. This systematic pre-submission methodology helps clinics address billing problems before they become revenue losses.
According to APTA's 2025 report, the established benchmark for PT claim denials averages 12.9% across the industry. Of those denied claims, 72.4% of PT providers file appeals, but only 49.3% of appeals ultimately succeed. In practical terms, roughly half of all denied claims become permanent revenue losses that predictive AI tools can help prevent by catching documentation and coding issues upstream.
Automated scheduling and patient retention
AI-driven scheduling tools use proven predictive algorithms to forecast cancellation likelihood, manage waitlists automatically, and deliver targeted reminders to reduce patient no-shows. Given that PT no-show rates can reach 73% according to the PLOS ONE study referenced above, even modest improvements in appointment adherence translate to meaningful revenue recovery and improved clinical outcomes.
Better scheduling adherence also means better patient outcomes in practice, because physical therapy depends on consistent, repeated visits to produce the demonstrated clinical results that established rehabilitation methodology requires.
Pro-tip
Don't just add AI to your clinic as another technology layer. Add measurable value instead. The best practice for AI implementation is selecting tools that remove friction from daily workflows without creating additional oversight requirements or asking clinical staff to learn a separate platform. The gold standard for AI in physical therapy is native EMR integration, where documentation, scheduling, and billing all flow through a single unified system.
FAQ
Will AI replace physical therapists?
No. AI cannot replicate the manual therapy skills, clinical reasoning, and therapeutic relationship that define a physical therapist's established scope of practice. A 2024 survey of 430 physical therapy professionals published in the peer-reviewed journal Healthcare found that 85.1% of respondents were eager to learn and use AI in their clinical practice. Only 30% expressed any concern about AI threatening their profession, which demonstrates broad professional confidence in AI as a complementary administrative tool.
Is AI documentation compliant?
Yes, provided the licensed clinician reviews and signs every note as established by regulatory standards. The provider remains legally and ethically responsible for the content of the medical record regardless of the methodology used to generate the initial draft. According to CMS guidelines, the person who signs the documentation attests to its accuracy and completeness. Clinicians evaluating AI documentation tools should verify that the system supports existing compliance workflows, maintains a clear audit trail, and does not introduce new clinical risk.
How does AI reduce billing denials in physical therapy?
Predictive analytics tools systematically flag documentation gaps, coding inconsistencies, and payer-specific rule violations before claims are submitted to insurance companies. According to APTA's 2025 Administrative Burden Report, the average PT claim denial rate is 12.9% across the industry. Of those denied claims, 72.4% of providers file formal appeals, but only 49.3% of those appeals succeed. In practical terms, a clinic that processes 1,000 claims per year and sees the industry-average denial rate would permanently lose revenue on approximately 37 claims annually. AI tools that catch these errors before submission help clinics protect their revenue cycle and reduce administrative hours spent on the appeals process.
What should clinics look for when evaluating AI tools?
Clinics should prioritize tools that integrate natively with their existing EMR rather than requiring a separate platform that fragments the clinical workflow. The following evaluation framework covers the essential criteria:
- Transparency: The tool should clearly show how clinical outputs are generated so that providers can independently verify accuracy before signing each document.
- Clinician control: All documentation must remain under the provider's direct review and final approval at every stage of the process.
- Workflow integration: The tool should eliminate steps in current workflows rather than adding new tasks that increase cognitive load on clinical staff.
- Data security: The system must meet established HIPAA requirements and clearly define its methodology for storing, processing, and retaining patient data.
- Published evidence: Look for peer-reviewed research or independently verified case studies demonstrating real-world clinical use and measurable outcomes.
How quickly can a clinic expect results from AI implementation?
Clinical evidence suggests that benefits emerge within the first month of consistent use. The JAMA Network Open study demonstrated statistically significant reductions in clinician burnout after just 30 days of ambient AI scribe use across multiple health systems. For scheduling and billing tools, clinics typically observe measurable improvements in no-show rates and denial rates within the first 60 to 90 days of consistent use across the full clinical team.
The determining factor for successful AI adoption in practice is consistent implementation by the entire clinical and administrative team rather than partial or pilot-only rollouts that limit the technology's demonstrated impact.


.png)